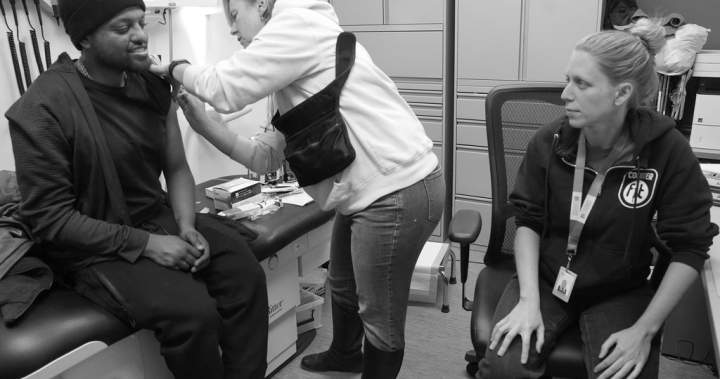
As the Ontario government cuts funding for seven supervised drug consumption sites in the province, workers at three remaining sites in Toronto that don’t rely on provincial funding say they’re worried the move will further strain their resources and lead to more overdoses and open drug use across the city.
The province said Monday it will initiate a 90-day wind-down period to give the seven defunded consumption sites time to transition to the government’s abstinence-based model — homelessness and addiction recovery treatment, or HART, hubs.
It said the move affects two sites in Toronto, two in Ottawa and one each in Niagara, Peterborough and London, with Health Minister Sylvia Jones saying in a statement that the government is “focused on treatment, recovery and safer communities.”
Health-care workers and harm reduction advocates have said the defunding would force these sites to close, leading to more overdoses and deaths.
In Toronto, the move likely means only three supervised consumption sites – Street Health, Casey House and the Kensington Market Overdose Prevention Site – would remain because they’re donor-funded.
Matt Johnson, an overdose prevention site supervisor at Street Health, says they were “not surprised, but horrified” by the province’s decision.
Johnson says the closure of two sites in the city means Street Health expects to see more people coming through its doors.
“Part of the reasoning behind having sites all over the city was so that no one site would be overly impacted. But if you take a bunch away, it means that the ones that are left have to pick up the slack and they get used more,” says Johnson.
“For those of us who work with this community and know these folks, it’s terrifying because we know the absolutely horrific impact it’s to have on the people who use these services.”
In 2024, Premier Doug Ford’s government banned consumption sites within 200 metres of a school or daycare, targeting 10 sites across the province for closure by the end of March 2025. Most of those sites chose to convert to the province’s abstinence-based model and closed. The government also banned new sites from opening.

Get weekly health news
Receive the latest medical news and health information delivered to you every Sunday.
After that move, Johnson says the number of people going to Street Health soared.
“We’ve already been feeling the impact of the closures that have already happened. Our numbers are way up, overdoses are way up. We are facing a need unlike anything we’ve seen in a long time,” Johnson says. “We’re a small site, we only have three booths. I don’t know how we’re going to address this.”
Though Street Health isn’t facing defunding after the province’s latest move, Johnson remains wary about the future of its overdose prevention site, given how the government “very clearly wants all the sites shut down.”
“On Monday, when our clients were first coming into the site, they were asking us questions about this and they were saying, ‘Is Street Health being shut down?’ And I kept saying, we are safe — for now. I can’t give anybody any assurances,” says Johnson.
“The other response I got was, ‘If they’re shutting all these places down, where do they expect us to go? And what do they expect us to do, just die?’”
Bill Sinclair, CEO of The Neighbourhood Group that runs the Kensington Market Overdose Prevention Site, says the two sites at Moss Park and Fred Victor that are set to be defunded are both far away from Kensington Market, so it’s unclear if their clients will travel to the remaining three sites or if it will result in more open drug use.
“I’m not sure whether people will make the trip, or in fact, they will just use unsafely, or as we’ve observed, people will start using (on public transit), people are using in public libraries,” Sinclair says.
The Kensington Market site remains open thanks to a court injunction last year following a Charter challenge. Still, it’s bracing for a jump in visitors in the fallout of the province’s latest decision, he adds.
“The smaller sites will do the best they can … this is not good health care. This is not how they should do it,” he says. “We’re grateful for our donors, but this is bigger than one or two charities can solve. We all need to get on the same page.”
Joanne Simons, CEO of Casey House, says her team was “devastated” to learn the province was defunding the seven sites. Casey House, which is also donor-funded, will likely see its resources stretched in the aftermath, she says.
“We anticipate that capacity will need to increase and our team is working on how we actually manage that,” says Simons, noting they’re currently assessing staffing needs and their hours of operation.
She’s also considering the “moral distress” the move could have on staff as they respond to increased demand, she says.
“Closing of the supervised consumption sites means that we are restricting access to a particular group of people. So how do we think about that from a human rights perspective?” she says.
Ford defended the decision to defund the provincially-supported sites earlier this week, claiming that unlike HART hubs, consumption sites “encourage” drug use.
“I don’t want to hurt these people. I want to help them. I want them to be productive,” Ford said Monday at an unrelated press conference, noting the province is investing $550 million in HART hubs.
But advocates say the defunding of consumption sites and their consequent closures will ultimately lead to more deaths. Janet Butler-McPhee, co-executive director of the HIV Legal Network, said last week that the province’s decision is a “cowardly move.”
“People will die without access to the life-saving care they receive at these sites. The sites exist within our communities and make them better and safer for everyone,” she said at a virtual press conference Friday.
Organizations including the Canadian Civil Liberties Association and Amnesty International have also condemned the move, calling on the Ontario government to reverse its decision.
Johnson says it’s a misconception that harm reduction advocates are opposed to treatment. Supervised consumption sites do more than just distribute safe supplies and prevent overdoses, Johnson says — they’re often a “home base” for their clients and a place to access health care without barriers.
“We all support people who want to stop or change their drug use. But those of us who work in the field understand that that is often a really long process that requires a lot of support,” says Johnson.
“What safe consumption sites do is … they make sure that people can stay alive during that process.”